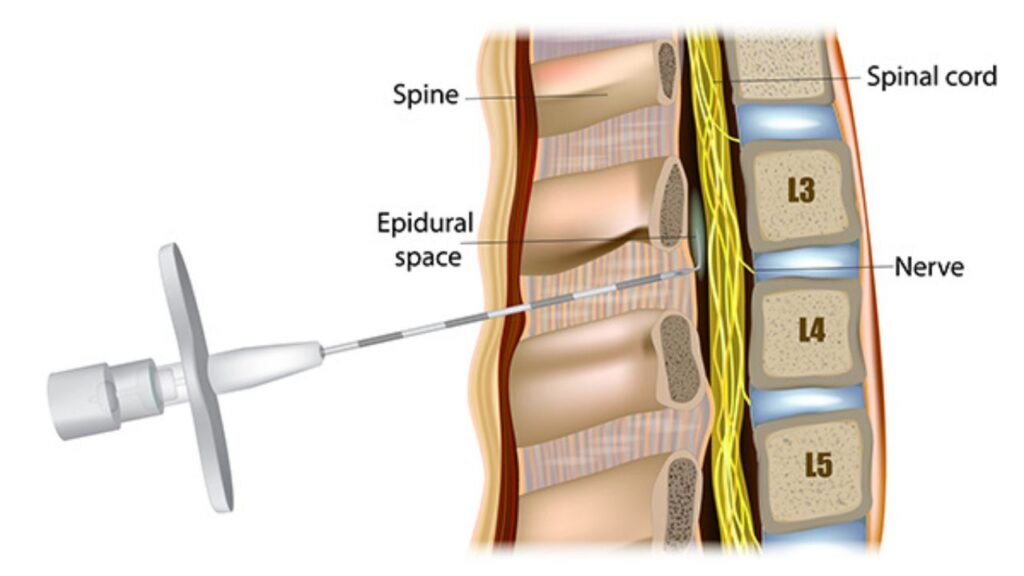
Yes, insurance firms often cover epidural injections, particularly for alleviating chronic pain in the lumbar spine region (lower back).
Nonetheless, coverage restrictions might apply to certain epidural injection types.
Consult your insurer to learn the precise policy details and the epidural injection varieties covered, as well as any stipulations.
Aspects that could influence coverage include epidural injection type, injection quantity, spinal area, and medical need.
How much is an epidural cost?
The cost for an epidural injection can fluctuate based on several factors like the kind of epidural, the site, and the supplier.
Uninsured individuals may pay anything from roughly $1,000 to above $8,000 for an epidural.
Can epidural injections be covered under both medical and dental insurance plans?
The coverage for epidural injections and insurance plans varies based on their type. Certain health insurance plans may include coverage for epidural injections used in chronic pain management or during childbirth.
However, it is important to verify the specifics and terms of your coverage by consulting your provider.
Dental insurance plans might cover certain dental procedures that necessitate anesthesia, although epidural injections may not fall under this category.
To find out the types of anesthesia covered and the corresponding circumstances, it is advisable to communicate with your dental insurance provider.
Are there any exclusions or limitations to epidural coverage in insurance policies?
Yes, there may be some exclusions or limitations to epidural coverage in insurance policies. Some possible exclusions or limitations are:
- A waiting period before you can claim epidural expenses.
- An upper limit on the amount of epidural expenses that can be reimbursed.
- A requirement of medical necessity for epidural injections.
- A lack of evidence for the effectiveness of epidural injections for certain conditions or beyond a certain duration.
- A preference for alternative treatments or conservative management before epidural injections.
You should read your insurance policy carefully and contact your insurance provider if you have any questions or doubts about your epidural coverage.
Does insurance typically provide coverage for epidural anesthesia during childbirth?
Indeed, many insurance policies cover epidural anesthesia in childbirth, given its widespread use for effective pain relief. Nonetheless, certain policies might impose conditions or restrictions on epidural coverage, including:
- Out-of-pocket copayments or deductibles.
- Preauthorization or referrals from primary care providers or obstetricians.
- Constraints on epidural anesthesia types (e.g., combined spinal-epidural or single-shot spinal) or the authorized provider.
- Limits on the duration or quantity of epidural anesthesia covered.
To determine your specific epidural coverage during childbirth and the necessary steps to obtain it, consult your insurance provider.
Can insurance companies deny coverage for epidurals based on specific medical conditions?
Yes, insurance companies may deny coverage for epidurals based on specific medical conditions. Some possible medical conditions that may affect epidural coverage are:
- Bleeding disorders or anticoagulant therapy increase the risk of bleeding complications.
- Infection at the site of injection or systemic infection increases the risk of infection complications.
- Allergy to local anesthetics or other components of the epidural solution that increase the risk of allergic reactions.
- Neurological disorders or spinal abnormalities that increase the risk of nerve injury or spinal headache.
- Severe hypotension or cardiovascular instability increases the risk of hemodynamic complications.